Guide on formula Feeding and Breaking the Top-Up Trap
Quick Answer
The “top-up trap” happens when formula feeding reduces your breastfeeding frequency, which then decreases your milk supply, leading to more formula - a difficult cycle to break. But it IS possible to wean your baby off formula and return to exclusive breastfeeding (sirf maa ka doodh). The key is: increase breastfeeding frequency to 10-12 times in 24 hours, ensure proper latching, and gradually reduce formula by 30-60ml every 3-4 days while monitoring baby’s weight and wet diapers.
Understanding the Top-Up Trap
Why Does This Happen?
Many new mothers fall into the top-up trap when formula is introduced for reasons like:
- “Baby isn’t getting enough milk” (often a misconception)
- “To give mother rest”
- “Until milk comes in properly”
- “Baby isn’t gaining weight fast enough”
- Latching difficulties
- Baby in NICU separated from mother
- Pressure from family or even some medical staff Often, these reasons are well-intentioned but not medically necessary.
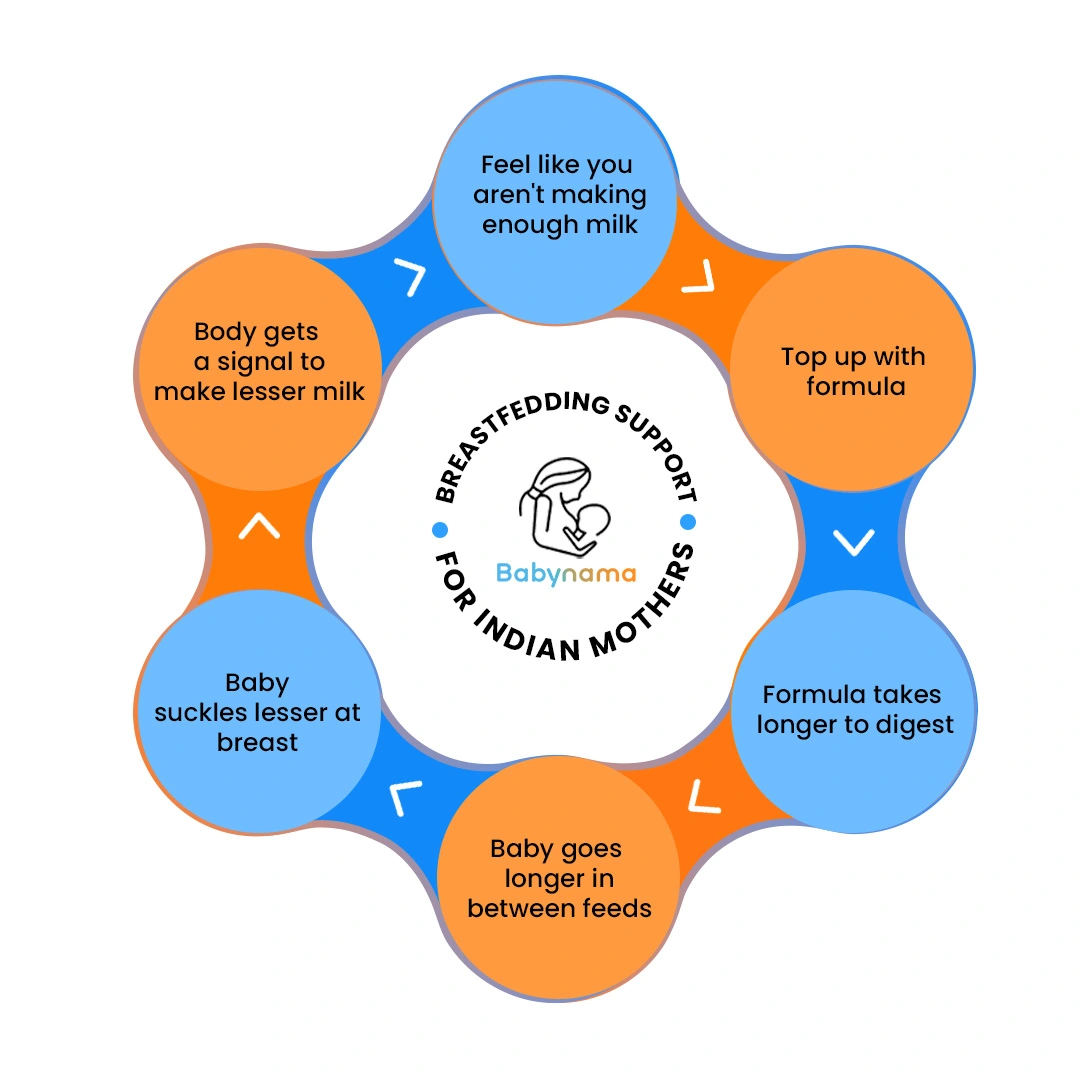
How the Trap Works
Breast milk production is based on demand and supply:
- Baby nurses at breast → Brain gets signal → Body makes more milk
- When baby takes formula → Baby skips a nursing session → Less demand signal
- Less demand → Body makes less milk → Baby needs more formula
- More formula → Even less nursing → Supply drops further
Reassurance: If you’re in this trap, please don’t feel guilty. You did what you thought was best. The good news is that it’s possible to break free at almost any stage.
Is Breaking the Top-Up Trap Right for You?
This guide is for you if:
-
You want to exclusively breastfeed
-
Your baby is healthy and gaining weight
-
You have support and can dedicate time to this process
-
Your milk supply hasn’t completely dried up This may not be suitable if:
-
Baby has specific medical conditions requiring formula
-
You’re on medications incompatible with breastfeeding
-
You’re unable or choose not to breastfeed

-
Your mental health is suffering from breastfeeding pressure Important: The goal is a happy, healthy mother and baby. If formula feeding works for your family, that’s completely valid too.
Step-by-Step Guide to Breaking the Top-Up Trap
Step 1: Get Professional Support
Before starting, consult with:
- A certified lactation consultant (IBCLC)
- Your pediatrician
- A breastfeeding support group They can help assess your specific situation and create a personalized plan.
Step 2: Assess Your Current Situation
Answer these questions:
- How many times do you breastfeed in 24 hours?
- How much total formula does baby take in 24 hours?
- Is baby latching correctly?
- What’s baby’s current weight trend? Tracking template:
| Time | Breastfed? | Duration | Formula given | Wet diaper? |
|---|---|---|---|---|
| 6 AM | Yes | 15 min | 30ml | Yes |
| … | … | … | … | … |
Step 3: Increase Breastfeeding Frequency
Target: 10-12 breastfeeding sessions in 24 hours
This is the most important step. Every time baby shows hunger cues:
-
Offer breast first - always
-
Let baby nurse as long as they want
-
Offer second breast after first is drained
-
Only then, if needed, offer formula as top-up Signs baby is hungry:
-
Rooting (turning head, opening mouth)
-
Hand to mouth movements
-
Fussiness
-
Lip smacking Don’t wait for crying - that’s a late hunger sign.
Step 4: Fix the Latch
A poor latch means baby isn’t effectively removing milk, which signals your body to make less.

Signs of good latch:
-
Wide open mouth around nipple AND areola
-
Lips flanged outward (fish lips)
-
Chin touching breast
-
Rhythmic suck-swallow-breath pattern
-
No pain for mother (mild tenderness initially is okay)
-
Audible swallowing If latching is difficult:
-
Try different positions (cradle, cross-cradle, football, side-lying)
-
Ensure baby’s nose, mouth, and chin are in line
-
Bring baby to breast, not breast to baby
-
Seek help from a lactation consultant
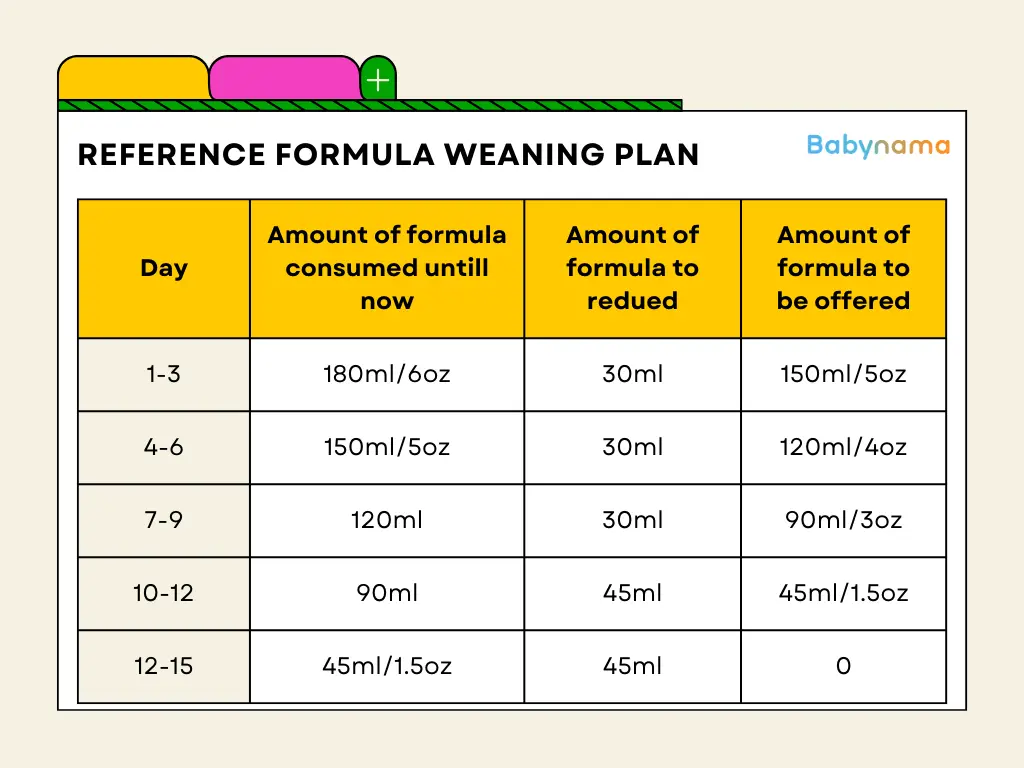
Step 5: Create Your Weaning Plan
Formula Weaning Schedule:
| Starting Formula | Reduction Plan |
|---|---|
| Less than 90ml (3oz) per day | May be able to stop quickly with increased nursing |
| 90-150ml (3-5oz) per day | Reduce 30ml every 3-4 days |
| 150-300ml (5-10oz) per day | Reduce 30-60ml every 3-4 days |
| More than 300ml per day | Reduce 60ml every 3-4 days, may take several weeks |
Example 15-Day Plan (for baby taking 210ml/day):
| Days | Formula Allowed |
|---|---|
| 1-4 | 180ml total |
| 5-8 | 120ml total |
| 9-12 | 60ml total |
| 13-15 | 0ml (only breast milk) |
Step 6: Monitor Baby Closely
Daily checks:
-
Wet diapers: At least 6 wet diapers per day
-
Poop: Regular stools (pattern varies by baby)
-
Alertness: Baby should be active and alert
-
Feeding behavior: Satisfied after feeds Weekly checks:
-
Weight gain (at least 150-200g per week initially) When to pause or slow down:
-
Fewer than 6 wet diapers
-
Baby seems constantly hungry
-
Weight gain stalling
-
Baby excessively fussy If these occur, return to previous formula level for a few more days before reducing again.
Techniques to Boost Milk Supply (Doodh Badhane Ke Upay)

Skin-to-Skin Contact (Kangaroo Care)
How it works:
-
Undress baby to diaper, place on your bare chest
-
Cover both with blanket
-
Do this for 1-2 hours daily, or more Why it helps:
-
Releases oxytocin (milk letdown hormone)
-
Baby roots and nurses more naturally
-
Strengthens breastfeeding relationship
-
Regulates baby’s temperature and heartbeat
Nursing Vacation
What it is:
A period (2-3 days) where you and baby stay together, focused almost entirely on breastfeeding.
How to do it:
- Clear your schedule
- Stay in bed or on couch with baby
- Do lots of skin-to-skin
- Nurse at every opportunity
- Have someone else handle everything else (cooking, cleaning, other children) This intensive period can dramatically boost supply.
Power Pumping
If baby isn’t nursing frequently enough:
Pump for:
- 20 minutes pumping
- 10 minutes rest
- 10 minutes pumping
- 10 minutes rest
- 10 minutes pumping Do this once daily, in addition to regular nursing/pumping.
Express Breast Milk (EBM) Instead of Formula
Progression:
- Initial: Breastfeed + EBM + Formula
- Middle: Breastfeed + EBM (less formula)
- Goal: Breastfeed + small EBM (no formula)
- Final: Breastfeed only Pump after nursing sessions to collect EBM for top-ups.
Traditional Galactagogues
Many Indian mothers use these to boost supply:
| Galactagogue | How to Use |
|---|---|
| Methi (fenugreek) | Methi ladoos, methi water, methi seeds in food |
| Saunf (fennel) | Saunf water, saunf seeds after meals |
| Jeera (cumin) | Jeera water, in cooking |
| Ajwain | In parathas, ajwain water |
| Dalia (broken wheat) | Dalia porridge daily |
| Dry fruits ladoos | Daily with milk |
Note: These work best when combined with frequent nursing. They alone cannot increase supply without the demand signal.
Important Techniques to Support the Process
Avoid Bottles (If Possible)
Bottles provide fast flow that can make babies prefer them over breast.
Alternatives for top-up:
- Katori-chamach (cup and spoon) - traditional Indian method
- Paladai (feeding cup)
- Syringe (without needle) along finger
- Small open cup
If You Must Use Bottles: Paced Bottle Feeding
- Use the slowest flow nipple
- Hold baby upright at 45 degrees
- Hold bottle horizontal, not tilted down
- Let baby suck milk out (don’t pour it in)
- Take breaks every few sucks
- Limit feeding to 10-15 minutes
- Stop when baby shows fullness signs This mimics breastfeeding rhythm and prevents overfeeding.
Offer Both Breasts Every Session
When building supply:
- Start on one breast, nurse until well-drained
- Switch to second breast
- If baby is still hungry, switch back to first
- Breast compression while nursing helps drain more milk
Avoid Pacifiers and Nipple Shields
While working to increase supply:
- Pacifiers satisfy sucking urge that could be used for nursing
- Nipple shields may reduce stimulation to your nipple Use these only if specifically recommended by your lactation consultant.
The WEANING Acronym
Remember this to stay on track:
W - Wean formula gradually (not suddenly)
E - Express and offer EBM as top-up
A - Attachment (latch) - ensure it’s correct
N - Nursing vacation - dedicate time to breastfeeding
I - Increase nursing frequency (10-12 times daily)
N - No to bottles (use cup/spoon instead)
G - Galactagogues (if needed, along with other efforts)
When Professional Help is Essential
Seek immediate help from a lactation consultant if:
- Baby is losing weight during this process
- You’re experiencing severe breast pain or infection
- Baby refuses the breast entirely
- Your mental health is suffering
- You’ve tried for 2 weeks without improvement
Expert Insight: Dr. Sumitra often reminds parents: ‘Breastfeeding is a skill that takes time to master. Don’t be hard on yourself.‘
FAQs
Q: My baby is 3 months old and has been on formula since week 1. Is it too late?
A: It’s not too late! Many mothers have successfully weaned from formula even after several months. The process may take longer, but your milk supply can be rebuilt. You may not achieve 100% breastfeeding, but even partial breastfeeding provides significant benefits.
Q: Will my baby lose weight when I reduce formula?
A: Slight weight gain slowdown is normal initially. However, if baby loses weight or has fewer than 6 wet diapers, return to previous formula amount. This is why gradual reduction and close monitoring are essential.
Q: My mother-in-law says my milk isn’t enough because baby cries after feeding. Is she right?
A: Babies cry for many reasons - not just hunger. Growth spurts, gas, need for comfort, overtiredness can all cause crying. If baby has 6+ wet diapers and is gaining weight, your milk is likely sufficient. The best response to cluster feeding (wanting to nurse frequently) is to nurse more - this builds supply.
Q: Can I take medication to increase milk supply?
A: Some medications (like domperidone) can help, but should only be used under doctor supervision due to side effects. Try non-medical methods first. If considering medication, consult your doctor and a lactation specialist.
Q: How long will it take to completely wean off formula?
A: It depends on how much formula baby is currently taking. For babies on 200-300ml daily, expect 2-4 weeks. For higher amounts, it may take 4-6 weeks or more. The key is patience and gradual reduction.
Q: What if I can’t completely eliminate formula?
A: Any amount of breast milk provides benefits. If you achieve 50% breastfeeding, that’s still 50% more than none! Don’t let perfection be the enemy of good. Combination feeding (breast milk + formula) is a valid choice.
This article was reviewed by a pediatrician and certified lactation consultant. Last updated: January 2025
Medical Advice Disclaimer: This information is for educational purposes. Always consult your healthcare provider before making changes to your baby’s feeding routine.
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!
Related Tools
Need Expert Breastfeeding Support?
Get personalized guidance from certified lactation consultants.
Explore Breastfeeding Program