Administering Insulin Injections for Children with Type 1 Diabetes
Quick Answer: Giving insulin injections to your child with Type 1 Diabetes can feel scary at first, but it becomes routine with practice. The key steps: choose the right site (tummy, thigh, or upper arm), pinch the skin, insert the needle at 90°, inject slowly, and hold for 10 seconds before removing. Rotate injection sites to prevent lumps. With proper technique and your pediatrician’s guidance, you’ll both become comfortable with this life-saving routine.
Understanding Type 1 Diabetes and Insulin
In Type 1 Diabetes (T1D), the body’s immune system destroys the insulin-producing cells in the pancreas. Without insulin, the body cannot use glucose for energy, causing blood sugar to rise to dangerous levels.
Why Insulin Injections Are Necessary
| Without Insulin | With Insulin |
|---|---|
| Blood sugar rises dangerously | Blood sugar stays controlled |
| Body cannot use food for energy | Body functions normally |
| Can lead to diabetic ketoacidosis | Prevents complications |
| Long-term organ damage | Healthy growth and development |
Reassurance: While managing T1D requires daily effort, children with diabetes can live full, active, healthy lives with proper insulin management.
What You’ll Need
Essential Supplies
| Item | Purpose |
|---|---|
| Insulin (as prescribed) | The medication |
| Insulin syringes or pen | Delivery device |
| Alcohol swabs | To clean injection site |
| Sharps container | Safe needle disposal |
| Blood glucose meter | Monitor sugar levels |
| Logbook or app | Track doses and readings |
Storage Tips
- Store unopened insulin in refrigerator (2-8°C)
- In-use insulin can be at room temperature (up to 28 days)
- Never freeze insulin
- Check expiry dates regularly
- Discard if insulin looks cloudy (unless it’s supposed to be)
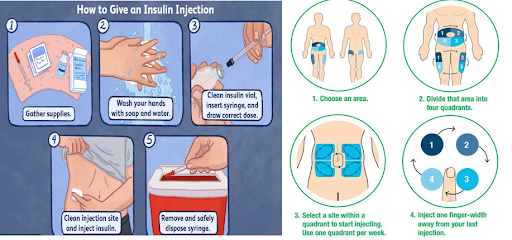
Step-by-Step Injection Guide
1. Preparation
- Wash hands thoroughly with soap and water
- Check insulin - correct type, not expired, looks normal
- If using cloudy insulin - gently roll between palms (don’t shake)
- Gather supplies - syringe/pen, alcohol swab, sharps container
2. Drawing Up Insulin (For Syringes)
- Clean the insulin vial top with alcohol swab
- Pull back plunger to draw air equal to dose needed
- Insert needle into vial, inject air
- Turn vial upside down
- Pull back plunger to draw correct dose
- Check for air bubbles - tap to remove, push out excess
3. Choosing Injection Site
Best Sites for Children:
| Site | Best For | Notes |
|---|---|---|
| Abdomen | Fastest absorption | Avoid 2 inches around belly button |
| Thighs | Easy for self-injection | Outer, front area |
| Upper arms | Good for thin children | Back of upper arm |
| Buttocks | Slowest absorption | Upper outer area |
4. Giving the Injection
- Clean the site with alcohol swab, let dry
- Pinch the skin gently to create a fold
- Insert needle at 90° angle (or 45° for thin children)
- Push plunger slowly and steadily
- Count to 10 before removing needle
- Release skin and remove needle straight out
- Apply gentle pressure - don’t rub
Site Rotation: Why It Matters
The Importance of Rotation
Injecting in the same spot repeatedly can cause:
- Lipohypertrophy - Hard lumps under skin
- Poor insulin absorption - Unpredictable blood sugar
- Skin damage - Scarring and discoloration
Rotation Pattern
Create a mental grid pattern:
- Divide each area into sections
- Move to new section each injection
- Don’t return to same spot for 1-2 weeks
- Keep a rotation log if helpful
Making Injections Easier for Children
For Younger Children
| Strategy | How It Helps |
|---|---|
| Let them choose the site | Gives sense of control |
| Use distraction | Videos, songs, counting |
| Praise and rewards | Positive reinforcement |
| Stay calm | Children sense your anxiety |
| Use numbing cream | EMLA cream 30 min before |
| Quick and confident | Don’t hesitate |
For Older Children
- Gradually teach self-injection
- Start with pushing the plunger while you hold
- Progress to choosing site and preparing
- Eventually, full independence with supervision
Goal: Most children can self-inject by age 8-10 with proper training and support.
Common Problems and Solutions
| Problem | Solution |
|---|---|
| Injection hurts | Use new needle each time, inject at room temperature |
| Bruising at site | Don’t inject into veins, apply pressure after |
| Lumps forming | Improve rotation, don’t use lumpy areas |
| Insulin leaking out | Count to 10 before removing needle |
| Child refuses | Take a break, offer choices, seek counseling if persistent |
When to Seek Help
Call Your Diabetes Team If:
- Blood sugar consistently too high or low
- Signs of infection at injection site
- Persistent lumps that don’t improve
- Child develops fear that interferes with treatment
- Any questions about dose or technique
Emergency Signs:
- Blood sugar very high (>300 mg/dL) with ketones
- Blood sugar very low (<70 mg/dL) and child can’t eat
- Confusion, extreme fatigue, vomiting
- Difficulty breathing
Frequently Asked Questions
Q: Can I use the same needle more than once?
A: It’s not recommended. Needles become dull after one use, making injections more painful and increasing infection risk. Always use a new needle.
Q: What if my child cries every time?
A: This is common initially. Stay calm, be quick and confident, offer comfort afterward. If it persists, ask your diabetes team about strategies or numbing cream.
Q: Can insulin be given through clothing?
A: It’s not recommended. While some do it in emergencies, it increases infection risk and makes site rotation harder to track.
Q: How do I handle injections at school?
A: Work with the school to create a diabetes management plan. A school nurse or trained staff can help, or older children can self-inject with supervision.
Q: What if I accidentally give too much insulin?
A: Give your child fast-acting sugar (juice, glucose tablets) and monitor closely. Call your diabetes team for guidance. Know the signs of low blood sugar.
Key Takeaways
- Proper technique - Pinch skin, inject at correct angle, count to 10
- Rotate sites - Prevents lumps and ensures proper absorption
- Stay organized - Keep supplies ready and track doses
- Make it routine - Same time each day helps both of you
- Empower your child - Gradual independence builds confidence
- Seek support - Your diabetes team is there to help
This article was reviewed by pediatricians at Babynama. Last updated: January 2026
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!
Related Tools