All About Childhood Asthma
Quick Answer
Yes, childhood asthma can be well-managed, and most children lead completely normal, active lives. Asthma is one of the most common chronic conditions in children (over 7 million children worldwide), but with proper treatment and trigger avoidance, your child can play sports, attend school regularly, and sleep peacefully through the night.

Why This Happens (Asthma Kyun Hota Hai)
Asthma is a condition where the airways in the lungs become inflamed and narrow, making breathing difficult.
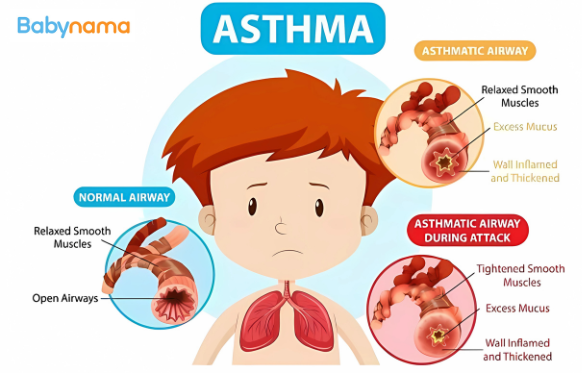
What happens during asthma:
- Airways swell up (inflammation)
- Muscles around airways tighten
- Extra mucus is produced
- Air can’t flow easily = wheezing, coughing, breathlessness Why some children get asthma:
| Risk Factor | Explanation |
|---|---|
| Family history | If parents have asthma/allergies, child is more likely to have it |
| Allergies | Eczema, food allergies, allergic rhinitis increase risk |
| Premature birth | Lungs may not be fully developed |
| Respiratory infections | Early severe infections can trigger asthma |
| Pollution exposure | Air pollution, smoking during pregnancy or around child |
| Obesity | Overweight children have higher risk |
Good news: Many children “outgrow” asthma or have much milder symptoms as they get older!
Age-Wise Understanding
| Age | Asthma Presentation | Special Considerations |
|---|---|---|
| Under 2 years | Wheezing with colds, recurrent bronchiolitis | Hard to diagnose definitively. May be called “reactive airway disease” |
| 2-5 years | Frequent coughing, especially at night. Wheezing | Can start formal diagnosis. Nebulizers often used |
| 5-12 years | Classic asthma symptoms. Can use inhalers | Peak flow monitoring possible. Sports participation important |
| Teenagers | May have less symptoms OR may worsen | Compliance can be an issue. Peer pressure, smoking risk |
Symptoms to Watch For (Lakshan)
Common signs of asthma:
-
Khansi (Coughing) - Especially at night, early morning, during exercise, or when laughing
-
Seeti ki awaaz (Wheezing) - Whistling sound when breathing out
-
Sans phoolna (Breathlessness) - Getting tired quickly during play
-
Seene mein jakdan (Chest tightness) - Child may say “chest feels heavy”
-
Raat ko khansi se uthna - Coughing that disturbs sleep (neend mein problem) Pattern recognition:
-
Symptoms worse at night or early morning
-
Symptoms triggered by exercise, cold air, smoke, dust
-
Symptoms improve with asthma medication
-
Family history of allergies/asthma
When to Worry (Emergency Signs) - Hospital Jayein
Call ambulance or rush to hospital if:
-
Very fast breathing - Nostrils flaring, ribs visible with each breath
-
Blue lips or fingernails - Not getting enough oxygen
-
Can’t speak in full sentences - Too breathless
-
Inhaler not helping - No improvement after using reliever inhaler
-
Hunched shoulders - Using neck/shoulder muscles to breathe
-
Drowsy or confused - Dangerous sign of low oxygen
-
Severe anxiety - Child is panicking, can’t calm down Urgent (same-day doctor visit):
-
Symptoms getting worse over days
-
Needing reliever inhaler more than usual
-
Night coughing increasing (raat ko bahut jagta hai due to cough)
-
Missing school due to symptoms
What You Can Do (Kya Karein)
1. Identify and Avoid Triggers
Common triggers in India:
| Trigger | How to Avoid |
|---|---|
| Dust mites | Wash bedding weekly in hot water, use mattress covers, reduce carpets |
| Pollution | Stay indoors on high AQI days, use air purifier, avoid traffic areas |
| Smoke | No smoking at home (even in other room!), avoid dhoop, agarbatti near child |
| Pollen | Keep windows closed during high pollen season |
| Pets | Keep pets out of bedroom, bathe them regularly |
| Cold air | Cover nose/mouth with muffler in winter |
| Exercise | Warm up slowly, take preventive puff if prescribed |
| Strong smells | Avoid phenyl, room fresheners, perfumes near child |
2. Medications - Understanding Them
Two types of asthma medicines:
1. Relievers (Emergency use - “rescue inhaler”)
-
Used during symptoms/attack
-
Works in minutes
-
Opens airways quickly
-
Examples: Salbutamol, Levosalbutamol
-
“Blue inhaler” in many countries 2. Controllers (Daily prevention)
-
Used EVERY DAY, even when feeling fine
-
Reduces inflammation
-
Prevents attacks
-
Takes weeks to show full effect
-
Examples: Inhaled corticosteroids (Budesonide, Fluticasone)
-
“Brown/orange inhaler” often Important: Controller medicines are NOT steroids that cause side effects like tablets. Inhaled steroids are safe for long-term use in children!
3. Using Inhalers Correctly
For children under 6: Use spacer + mask
-
Shake inhaler
-
Attach to spacer
-
Place mask on child’s face
-
Press inhaler once
-
Let child breathe normally 5-6 breaths
-
Wait 30 seconds, repeat if needed For children 6+: Spacer without mask
-
Shake inhaler
-
Attach to spacer
-
Child breathes out fully
-
Seals lips around spacer mouthpiece
-
Press inhaler, breathe in slowly
-
Hold breath 10 seconds
-
Breathe out slowly Common spacers available in India: Zerostat, Aerochamber, Babyhaler
4. Creating an Asthma Action Plan
Work with your doctor to create a written plan:
| Zone | Symptoms | Action |
|---|---|---|
| Green (All clear) | No symptoms, sleeping well, can play | Continue controller medicines |
| Yellow (Caution) | Some coughing/wheezing, waking at night, using reliever more | Increase controller as per plan, avoid triggers |
| Red (Emergency) | Severe breathlessness, reliever not helping | Use reliever, call doctor/go to hospital |
5. Lifestyle Management
Sleep tips (Neend ke liye):
-
Keep bedroom dust-free
-
Wash bedding in hot water weekly
-
No stuffed toys on bed
-
Elevate head slightly
-
Use air purifier if possible
-
Keep bedroom cool but not cold Exercise:
-
Asthma should NOT stop your child from playing
-
Warm up before exercise
-
Use preventive puff if prescribed
-
Carry reliever inhaler to sports
-
Swimming is excellent for asthmatic children
-
Avoid exercising in very cold or polluted air Diet:
-
No specific “asthma diet”
-
Balanced nutrition supports immune system
-
Some children have food triggers (rare) - keep a diary
-
Maintain healthy weight
Frequently Asked Questions
Q: Mera bachcha raat ko bahut khaans-ta hai aur uth jaata hai. Kya yeh asthma hai?
A: Night coughing that disturbs sleep is a classic sign of asthma, especially if it happens regularly. Other causes include post-nasal drip, reflux, or just a lingering cold. If night coughing is frequent (raat ko jagta hai regularly) and you notice wheezing or breathlessness, consult a pediatrician. A proper evaluation can confirm if it’s asthma.
Q: Inhaler ki aadat pad jaati hai kya? Ek baar shuru kiya toh band nahi hoga?
A: This is a very common myth. Inhalers are NOT addictive. Asthma is a chronic condition that needs management - stopping the inhaler doesn’t cure asthma, it just removes the treatment. Many children can reduce or stop controller medication over time as their asthma improves, under doctor’s guidance. Using inhaler properly is BETTER than avoiding it and having frequent attacks.
Q: Steroid inhaler safe hai bacchon ke liye?
A: YES! Inhaled steroids are very safe. The dose is very small, and it goes directly to the lungs - very little is absorbed into the body. The small amount that might be absorbed is much safer than the alternative: uncontrolled asthma, frequent oral steroids, emergency visits, and damaged lungs. Decades of research confirm inhaled steroids are safe for long-term use in children.
Q: Baccha sports khel sakta hai asthma hone ke baad?
A: Absolutely! Many Olympic athletes have asthma. With good asthma control, your child should have NO limitations on physical activity. In fact, exercise is GOOD for asthmatic children - it strengthens lungs. Just ensure proper warm-up, carry reliever inhaler, and if prescribed, use preventive puff before exercise.
Q: Nebulizer better hai ya inhaler?
A: Inhalers with spacer are actually BETTER than nebulizers for most situations! They’re faster, portable, and deliver medicine more effectively. Nebulizers are useful when child is too young or too sick to use an inhaler, or during severe attacks. Don’t think nebulizer is “stronger” - same medicine, just different delivery method.
Q: Pollution season mein bachcha bahut beemar hota hai. Kya karein?
A: Delhi’s pollution season is tough for asthmatic children. Keep child indoors when AQI is very high. Use N95 mask when going out. Use air purifier at home. Increase controller medication dose (as per doctor’s advice) during high pollution days. Keep windows closed. Do indoor activities instead of outdoor play. Monitor symptoms closely.
Q: Asthma theek ho jayega bachpan ke baad?
A: Many children do “outgrow” asthma - symptoms decrease significantly or disappear by teenage years. However, it varies - some continue to have asthma, and some may have it return in adulthood. You can’t predict for sure. Focus on good control now - well-controlled asthma has better long-term outcomes.
This article was reviewed by a pediatrician. Last updated: January 2025
Worried about your child’s coughing or breathing? Babynama’s pediatricians can help assess symptoms, create an asthma action plan, and guide you through managing your child’s asthma. Chat with us on WhatsApp!
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!
Related Tools