All About Childhood Asthma: Causes, Symptoms, and Management
Quick Answer
Yes, childhood asthma is manageable and most children live completely normal, active lives! Asthma affects over 7 million children globally and typically begins before age 5. With proper medication and trigger avoidance, your child can play sports, sleep through the night (achhi neend), and attend school regularly without problems.

What Causes Childhood Asthma
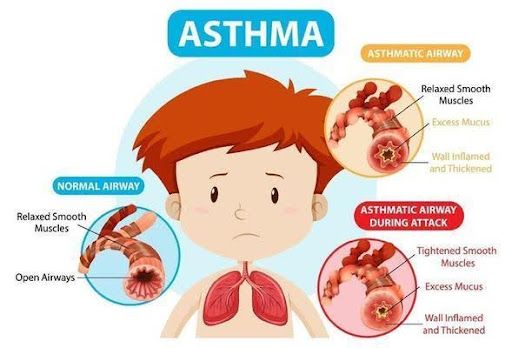
Asthma is a chronic lung condition where airways become inflamed and narrow, making breathing difficult.
What happens in asthma:
- Airways swell (soojhan)
- Muscles around airways tighten
- Extra mucus (balgam) is produced
- Air can’t flow properly = wheezing, coughing Risk factors (Kisko zyada risk hai):
| Risk Factor | Explanation |
|---|---|
| Family history | If parents have asthma/allergies |
| Allergies | Eczema, food allergies, hay fever |
| Premature birth | Lungs may not be fully developed |
| Pollution exposure | Air pollution, smoking around child |
| Obesity | Overweight children have higher risk |
| C-section delivery | Some studies show slightly higher risk |
Good news: Many children’s asthma improves significantly or disappears as they grow older!
Symptoms to Watch For (Lakshan)
Classic asthma symptoms:
- Khansi (Cough) - Especially at night, early morning, during exercise
- Seeti ki awaaz (Wheezing) - Whistling sound when breathing
- Sans phoolna (Breathlessness) - Getting tired quickly during play
- Seene mein jakdan (Chest tightness) - Child says “chest feels heavy”
- Raat ko khansi - Cough that disturbs sleep (neend kharab) Severity levels:
| Severity | Signs | Impact on Daily Life |
|---|---|---|
| Mild | Occasional cough/wheeze | No sleep disturbance, can play normally |
| Moderate | Regular symptoms, night waking | Raat ko jagta hai, can’t run around easily |
| Severe | Daily symptoms, very breathless | Can’t sleep, can’t eat/talk, very tired |
Home Management (Ghar Pe Kya Karein)
Trigger Avoidance (Sabse Zaroori)
| Trigger | How to Avoid |
|---|---|
| Dust mites | Wash bedding weekly in hot water, use mattress covers |
| Pollution | Stay indoors on bad AQI days, use air purifier |
| Smoke | No smoking at home, avoid agarbatti/dhoop near child |
| Cold air | Cover nose/mouth with muffler in winter |
| Strong smells | Avoid phenyl, room fresheners near child |
Environment Optimization
- Keep bedroom clean and dust-free
- Remove carpets if possible
- No stuffed toys on bed
- Keep pets out of bedroom
- Use air purifier during pollution season
Lifestyle Tips
- Regular exercise - Swimming is excellent for asthmatic children
- Maintain healthy weight
- Stay hydrated
- Good sleep hygiene - Consistent bedtime routine
When to See a Doctor
EMERGENCY - Go to hospital immediately if:
-
Very fast breathing, ribs visible with each breath
-
Blue lips or fingernails
-
Can’t speak in full sentences
-
Inhaler not helping
-
Child is drowsy or confused
-
Severe panic/anxiety Schedule appointment if:
-
Symptoms getting worse over days
-
Needing reliever inhaler more than usual
-
Night coughing increasing
-
Missing school due to symptoms
-
Symptoms affecting daily activities
Treatment Options (Ilaaj)
Medications
1. Relievers (Emergency/Rescue)
-
Used during symptoms
-
Works in minutes
-
Opens airways quickly
-
Examples: Salbutamol (Asthalin), Levosalbutamol 2. Controllers (Daily Prevention)
-
Used EVERY DAY even when feeling fine
-
Prevents attacks
-
Takes weeks to show full effect
-
Examples: Budesonide, Fluticasone (inhaled steroids)
Delivery Devices
| Device | Best For | Notes |
|---|---|---|
| MDI with Spacer + Mask | Children under 6 | Most effective method |
| MDI with Spacer | Children 6+ | Child breathes through mouthpiece |
| Nebulizer | Very young/sick children | Same medicine, different delivery |
| Dry Powder Inhaler | Older children | Requires good coordination |
Common spacers in India: Zerostat, Aerochamber, Babyhaler
Prevention
You can’t prevent asthma, but you can prevent attacks:
- Take controller medicine daily as prescribed
- Avoid known triggers
- Keep rescue inhaler always available
- Have an Asthma Action Plan from doctor
- Get flu vaccine yearly
- Don’t stop medicines without doctor’s advice
Frequently Asked Questions
Q: Bachcha raat ko bahut khaans-ta hai aur jagta hai. Kya yeh asthma hai?
A: Night coughing (raat ko khansi) that regularly disturbs sleep is a classic sign of asthma. If it happens frequently and you notice wheezing or breathlessness too, consult a pediatrician for evaluation. Other causes include post-nasal drip or acid reflux, so proper diagnosis is important.
Q: Inhaler lene se aadat pad jaati hai kya?
A: Bilkul nahi! This is a very common myth. Inhalers are NOT addictive. Asthma is a chronic condition that needs ongoing management. Stopping inhaler doesn’t cure asthma - it just removes the treatment. Many children reduce or stop medicines as they grow, under doctor’s guidance.
Q: Nebulizer better hai ya inhaler?
A: Actually, inhalers with spacer are BETTER than nebulizers for most situations! They’re faster, portable, and deliver medicine more effectively. Nebulizers are useful for very young children or during severe attacks. Same medicine, just different delivery method.
Q: Kya asthmatic bachcha sports khel sakta hai?
A: Absolutely YES! Many Olympic athletes have asthma. With good control, your child should have NO limitations. Swimming is actually excellent for asthmatic children. Just ensure proper warm-up and carry reliever inhaler.
Q: Steroid inhaler safe hai bacchon ke liye?
A: Yes! Inhaled steroids are very safe - the dose is tiny and goes directly to lungs. This is very different from oral steroids. Decades of research confirm they’re safe for long-term use in children.
This article was reviewed by a pediatrician. Last updated: January 2025
Concerned about your child’s breathing or cough? Babynama’s pediatricians can help evaluate symptoms and create an asthma management plan. Chat with us on WhatsApp!
Need personalized guidance? Book a consultation with our pediatricians or explore our Care Plans for 24/7 expert support!
Related Tools