Quick Answer: What to Expect in the First 6 Weeks
Physical:
- Vaginal bleeding (lochia) for 4–6 weeks, heaviest in the first week
- Uterine cramping as the uterus contracts back to size, especially while breastfeeding
- Perineal soreness (vaginal birth) or wound tenderness (C-section) for 2–6 weeks
- Breast engorgement and nipple tenderness as milk comes in (days 2–5)
- Extreme fatigue — normal and expected
Emotional:
- Baby blues (weepiness, mood swings) in 70–80% of women, days 2–10, then resolving
- Postpartum depression in 10–15% of women — does not resolve on its own, needs help
- A strange mix of love, overwhelm, inadequacy, and isolation — all normal
Practical:
- First postpartum visit with your doctor at 6 weeks (earlier if complications)
- No sex or tampons until 6-week clearance (earlier if medically indicated)
- Most physical restrictions lift at 6 weeks, some C-section restrictions extend to 12 weeks
First 24 Hours After Birth
Vaginal birth
Immediately after delivery, the body begins its recovery. You will experience:
- Lochia: Vaginal bleeding that is heavier than a period, bright red, with possible clots. This is normal. A clot the size of a plum occasionally is normal. Clots larger than your fist, or soaking a pad in less than an hour for 2+ consecutive hours, need urgent evaluation.
- Perineal care: If you had a tear or episiotomy, keep the area clean. Use a peri-bottle with warm water after urination. Sitting on an ice pack for the first 24 hours reduces swelling. Salt baths help after the first 24 hours.
- The first urination: May be difficult due to swelling. Tell the nurse if you cannot urinate within 4–6 hours of delivery.
Skin-to-skin contact immediately after birth — placing the unclothed baby on your bare chest — has well-documented benefits: it stabilises the baby’s temperature, heart rate, and blood glucose, and helps establish breastfeeding. Hospitals increasingly support this; advocate for it if not offered.
Breastfeeding initiation: The colostrum (first milk) is available from birth and is the most nutrient-dense substance a newborn can receive. Put the baby to the breast within the first hour. Colostrum is thick and yellow — and produced in very small amounts (a teaspoon per feed is normal and sufficient for a newborn’s stomach, which is the size of a marble). Do not supplement with formula because the baby “isn’t getting enough” unless there is a medical indication.
C-section birth
After a Caesarean, you are in a surgical recovery ward for 1–4 hours before returning to your room. You will have:
- A urinary catheter (removed 12–24 hours post-surgery)
- IV fluids for the first 12–24 hours
- A wound dressing on the incision
- An epidural or spinal block wearing off over 2–4 hours — you will regain sensation gradually
Skin-to-skin is possible after a C-section — ask for it in the operating theatre if you are stable and the baby is well. “Natural Caesarean” practices that allow skin-to-skin on the operating table are increasingly offered.
The first stand: You will be encouraged to stand and take a few steps within 12–24 hours of surgery. This is important to prevent blood clots. It will feel difficult and frightening. Do it slowly, with support.
First Week at Home
Physical recovery: vaginal birth
- The first bowel movement: may take 2–4 days. Constipation is extremely common due to dehydration, iron supplements, and pain-avoidance behaviour. Drink plenty of water, eat fibre-rich foods (dal, fruit, vegetables), and take a stool softener if recommended. Do not strain.
- Episiotomy/tear care: keep dry after the peri-bottle rinse. Stitches dissolve on their own over 3–6 weeks. Slight discharge is normal; foul smell or significant spreading redness is not (potential infection).
- Haemorrhoids (piles): extremely common after vaginal birth. Sitz baths, witch hazel pads, and OTC haemorrhoid cream help. They typically resolve in a few weeks.
Physical recovery: C-section
- Wound care: Keep the incision dry for 24–48 hours after the dressing is removed. Clean gently with mild soap and water, pat dry. No scrubbing, no creams on the wound until fully healed (typically 2–3 weeks).
- Activities: Walking from day 2 (short distances, at home). No lifting anything heavier than your baby for 4–6 weeks. No driving for at least 4–6 weeks (you need to be able to perform an emergency stop).
- Wind pain: Trapped gas pain (shoulder tip pain, abdominal bloating) is common in the first 3–5 days after C-section. Walking, gentle movement, and warm compresses help.
Breast changes in the first week
- Milk typically “comes in” on days 2–5. The breasts become very full, hard, and tender (engorgement). This can temporarily feel like the baby cannot latch.
- Feed frequently and on demand — this is the best relief for engorgement and establishes supply.
- Warm compress before feeding to let milk flow; cool compress after feeding to reduce swelling.
- If the breast is stone-hard and the areola is too firm for the baby to latch, hand-express a little milk first to soften the nipple area.
The emotional first week
The first week is dominated by sleep deprivation, physical discomfort, and a profound shift in identity. Many women feel overwhelmed and wonder if they made a mistake. This does not mean you are a bad mother. It means you are adjusting to the biggest life change there is.
Baby blues: Weepiness, irritability, anxiety, and mood swings in the first 2 weeks. Affects 70–80% of mothers. It peaks around day 3–5 (when milk comes in and oestrogen drops sharply) and resolves on its own by 2 weeks. If low mood persists beyond 2 weeks or is severe, it is postpartum depression.
The Chilla: Evidence-Based vs Cultural
The “chilla” or “sacha” — 40 days of postpartum confinement — is practised across South Asia, with specific forms in North Indian, South Indian, and Muslim families. The principle is that the new mother rests, is cared for by family, and focuses on the baby. The duration varies by tradition from 30 to 40 days.
What is actually beneficial
- Rest: The postpartum period is physically demanding. Having family take over cooking, cleaning, and household tasks so the mother can sleep and feed the baby is genuinely helpful. Sleep deprivation is the single biggest driver of postpartum depression.
- Social support: Women with strong social support networks have lower rates of postpartum depression. Being cared for, not isolated, matters.
- Warm, high-calorie foods: The traditional emphasis on ghee, ajwain, dry fruits, and warm food makes nutritional sense — a new mother needs iron, calcium, and calories for breastfeeding.
- Reduced external obligations: 40 days without having to host, socialise, or function professionally is protective.
What is not evidence-based (or is actively harmful)
- Restricting fluid intake: Some traditions advise limited water and cold drinks. Adequate hydration is essential for breastfeeding. Drink as much as you feel you need.
- Oil massages on the wound: Applying oil or traditional preparations to a healing C-section wound before it is fully healed can cause infection.
- Extreme dietary restriction: Some chilla diets exclude entire food groups on the belief they cause “cold” or “gas” in the baby. There is no evidence that the mother’s diet (apart from known allergens like cow’s milk in rare cases) significantly affects breastfed babies’ gas. Eat a varied, nutritious diet.
- Complete confinement to one room: Fresh air and short walks improve mood, prevent blood clots, and promote healing. Short gentle walks from the first week (sooner with vaginal birth, slightly later with C-section) are beneficial.
- Not showering: No medical reason to avoid bathing postpartum. Hygiene reduces infection risk. Use warm water and keep the wound dry.
The chilla, in its protective-rest intent, is valuable. Apply it flexibly: take the rest and support, leave the restrictions that have no basis.
C-Section Recovery: Week by Week
Week 1
- Managed in hospital for 2–4 days typically
- Pain at wound site, managed with paracetamol and ibuprofen (if not contraindicated, and safe with breastfeeding)
- Short walks in the ward from day 2
- Wound dressing change before discharge; staples/clips removed at 5–7 days if non-dissolving sutures
Weeks 2–3
- Pain significantly reduced; some pulling or itching at incision (normal healing)
- Can walk around the home; climb stairs slowly
- No lifting beyond the baby
- Continue wound care: clean, dry, no creams until fully healed
- Some women experience numbness at and above the scar (nerves take months to recover)
Week 4–6
- Most functional recovery complete; wound is healing well
- Light activities at home: cooking, short errands
- Still no heavy lifting, strenuous exercise, or driving
6–12 weeks
- Medical clearance at 6-week visit
- Can start light exercise (walking, gentle yoga, pelvic floor)
- Driving typically cleared at 6 weeks if you can do an emergency stop without pain
- Sex: medically after 6-week clearance, but emotionally and physically many women are not ready for several more weeks — this is entirely normal
C-section scar care (from 6 weeks onwards)
Once the scar is fully healed (no scab, no open areas), scar massage improves the appearance and reduces the likelihood of internal adhesions. Use a neutral oil (coconut, almond) and massage the scar gently in circular motions for 5 minutes daily. This also helps with the numbness above the scar.
Postpartum Depression vs Baby Blues
Baby blues
- When: Days 2–10 after birth
- What it feels like: Weepiness, mood swings, irritability, feeling overwhelmed. You may cry for no clear reason.
- How long: Resolves on its own within 2 weeks
- What helps: Rest, support, reassurance
Postpartum Depression (PPD)
- When: Can start anytime in the first year, but typically within 3 months of birth
- What it feels like: Persistent low mood, inability to feel pleasure, withdrawing from the baby, feelings of worthlessness or guilt, difficulty bonding, recurrent dark thoughts, inability to sleep even when the baby sleeps
- How long: Does not resolve on its own. It is a medical condition.
- Prevalence: 10–15% of mothers. In India, studies suggest 20–25% due to social factors (gender disappointment, family pressure, financial stress, unsupportive partners).
The Edinburgh Postnatal Depression Scale (EPDS)
This is a validated 10-question screen used worldwide to identify PPD. Key questions include:
- “I have been able to laugh and see the funny side of things” (scoring reversed)
- “I have blamed myself unnecessarily when things went wrong”
- “I have felt scared or panicky for no very good reason”
- “The thought of harming myself has occurred to me”
A score of 12 or above suggests PPD. A “yes” to any question about self-harm requires immediate help. Ask your OB or pediatrician for the full EPDS scale at your 6-week visit.
PPD in India: the stigma problem
In India, PPD is dramatically under-diagnosed and under-treated. Cultural expectations that motherhood is naturally blissful, the belief that expressing negative feelings brings shame to the family, and the lack of awareness among both families and healthcare providers mean many women suffer in silence for months or years.
PPD is not: Weakness. Inability to cope. Bad motherhood. Lack of love for the baby.
PPD is: A medical condition caused by hormonal and neurological changes, exacerbated by sleep deprivation, pain, and social pressures, and treatable with therapy and/or medication.
Treatment options:
- Counselling/therapy: Cognitive Behavioural Therapy (CBT) has the strongest evidence for PPD. Seek a clinical psychologist with perinatal experience.
- Medication: SSRIs (sertraline, escitalopram) are safe in breastfeeding. This is a decision made with your doctor — medication is not automatically necessary but is not something to refuse out of fear.
- Support groups: Urban India has a small but growing network of PPD support groups, including online communities.
If you are in a crisis or having thoughts of harming yourself or your baby, call iCall (9152987821) or Vandrevala Foundation (1860-2662-345, 24 hours).
Postpartum Anxiety
Postpartum anxiety (PPA) is less talked about than PPD but may be equally common. It manifests as:
- Persistent worry that something terrible will happen to the baby
- Being unable to sleep even when the baby is sleeping, due to intrusive anxious thoughts
- Checking on the baby constantly
- Avoiding situations out of fear
- Physical symptoms: racing heart, shortness of breath, feeling on edge
Many mothers with PPA are told they are “being overprotective” or are “new mother nerves.” PPA, like PPD, is a diagnosable condition that responds to therapy and sometimes medication. If anxiety is significantly affecting your quality of life, seek help.
Physical Changes After Birth
Hair loss (telogen effluvium)
Between 2 and 5 months postpartum, most women notice dramatic hair shedding. This is telogen effluvium — during pregnancy, high oestrogen levels kept hair from shedding normally. After birth, oestrogen drops sharply and all that retained hair sheds at once.
It can be alarming — clumps in the shower, on the pillow, on the brush. It is almost always temporary. Hair growth returns to normal by 12 months postpartum in most women. Iron deficiency (common postpartum) can worsen hair loss — get your haemoglobin checked at the 6-week visit.
There is no evidence that any shampoo, oil, or supplement reverses telogen effluvium. Iron supplementation helps if you are deficient. Patience is the main treatment.
Diastasis recti
During pregnancy, the two columns of abdominal muscle (rectus abdominis) separate along the midline to accommodate the growing uterus. This separation — diastasis recti — is present to some degree in most women after pregnancy.
How to self-check: Lie on your back with knees bent. Lift your head slightly off the floor (like the beginning of a crunch). Press your fingers into the midline of your abdomen, just above and below the navel. A gap of more than 2 finger-widths that feels soft and unsupported is significant diastasis.
Diastasis recti causes: the characteristic “mummy tummy” pooch that does not respond to exercise, lower back pain, poor core stability, and sometimes urinary leakage.
What helps: Specific rehabilitation with a women’s health physiotherapist. General core exercises (particularly crunches, sit-ups, and planks) can make diastasis worse. Do not start abdominal exercises before getting a professional assessment if you suspect diastasis.
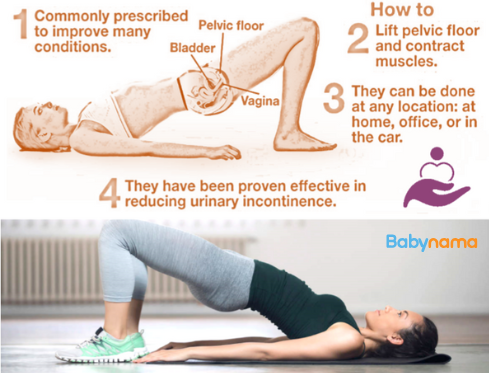
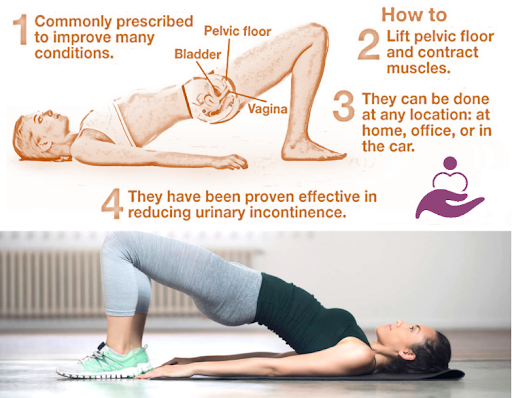
Pelvic floor dysfunction
The pelvic floor — a hammock of muscles supporting the bladder, bowel, and uterus — is stretched and sometimes damaged during vaginal birth. Consequences include:
- Stress urinary incontinence: Leaking urine with coughing, sneezing, jumping. Affects 30–50% of women postpartum.
- Pelvic organ prolapse: A feeling of heaviness or a bulge in the vaginal area. Mild prolapse is common; severe prolapse needs specialist input.
- Pain with sex
Pelvic floor exercises (Kegels): Contract the muscles you would use to stop urination. Hold for 5–10 seconds, release fully. Repeat 10 times, 3 times a day. Start from the first postpartum day (or as soon as the perineum is comfortable enough). These exercises are safe after both vaginal and C-section birth.
Important: Pelvic floor exercises are not enough for everyone. If symptoms are significant, see a women’s health physiotherapist (pelvic floor PT). In India, awareness of pelvic floor PT is low but services exist in major cities.
Postpartum Nutrition
Your body has just undergone significant blood loss and physical work. Breastfeeding requires approximately 400–500 extra calories per day. This is not the time for restrictive eating.
Focus areas
- Iron: Replace blood loss with iron-rich foods — ragi, dal, green leafy vegetables paired with Vitamin C. If haemoglobin is low at delivery, your doctor may prescribe iron supplements for 3–6 months. Take them.
- Calcium: Breastfeeding draws calcium from the mother’s bones. Maintain high calcium intake — ragi, dahi, paneer, til.
- Protein: Needed for tissue repair and breast milk production. 80–85 g protein/day during breastfeeding. Dal, paneer, eggs, chicken, dahi at every meal.
- Hydration: Drink to thirst — approximately 2.5–3 litres per day when breastfeeding. Coconut water, lassi, dal, soups all count.
Traditional postpartum foods that make sense
- Ajwain (carom seeds): carminative, helps with post-delivery gas pain, anti-inflammatory
- Methi ladoo / ajwain ladoo: calorie-dense, warming, iron-containing
- Dry fruit pinnis and panjiri: calorie-dense, mineral-rich — useful for a breastfeeding mother needing extra calories
- Jeera water: mild digestive aid
- Haldi (turmeric) in warm milk: anti-inflammatory, genuinely useful in wound healing
The traditional Indian postpartum kitchen, stripped of its unnecessary restrictions, is actually quite good nutritionally.
Returning to Exercise
Before 6 weeks
- Gentle walks from week 1 (vaginal birth) or week 2 (C-section)
- Pelvic floor exercises from day 1 or as soon as comfortable
- No impact activities, no swimming (open wound risk), no heavy lifting
At and after 6 weeks
Start with pelvic floor rehabilitation and diastasis assessment before returning to any abdominal or high-impact exercise.
Sequence:
- Pelvic floor rehabilitation (Kegels progressing to functional exercises) — weeks 6–12
- Core rehabilitation: breathing exercises, diaphragm engagement, transverse abdominis activation — weeks 6–12
- Walking progressing to brisk walking — from 6 weeks
- Yoga and Pilates (avoiding deep twists and strong inversions initially) — from 8–10 weeks
- Swimming — from 8–10 weeks (once wound fully healed)
- Light weight training — from 12 weeks
- Running, HIIT, heavy weights — not before 12–16 weeks, and only after pelvic floor clearance
The problem with rushing: Returning to high-impact exercise before the pelvic floor has recovered is the single most common cause of long-term prolapse and incontinence. A 12-week return to running programme is not slow — it is appropriate. Your body spent 40 weeks changing; it needs time to change back.
Going Back to Work in India
Your legal entitlement
The Maternity Benefit (Amendment) Act, 2017 provides:
- 26 weeks of paid maternity leave for the first two children (for women employed with establishments of 10 or more workers)
- 12 weeks for the third child onwards
- 12 weeks for adoptive and commissioning mothers (surrogacy)
- Work from home provisions at the employer’s discretion after maternity leave
- Crèche facility mandatory for establishments with 50 or more employees
This is not a favour from your employer — it is your legal right under Indian law.
Returning earlier than 26 weeks
Many women feel pressured (or are financially required) to return before their leave is up. If you are breastfeeding and returning to work:
- Establish pumping before you return (start 2 weeks before your return date)
- Build a milk stash of 1–2 days’ worth
- At work, pump every 3 hours to maintain supply
- Your employer is legally required to provide facilities under the Maternity Benefit Act — a clean room, not a toilet
The emotional weight of return
Many Indian mothers feel profound guilt about returning to work, regardless of whether it is by choice or necessity. This guilt is real and common. It does not mean you are harming your child. Babies with working mothers do not have worse outcomes; they often have mothers who model professional identity and independence.
Relationship Changes After Birth
Partner dynamics
The arrival of a baby almost always disrupts the couple relationship, even when both partners are prepared. Common sources of conflict:
- Division of night duties (who gets up, how often)
- Grandparent involvement and conflicting advice
- One partner feeling left out of the mother-baby bond
- Financial stress, especially if one partner has stopped working
- Different parenting philosophies that were not resolved before birth
None of this is evidence of a failing relationship. Studies show marital satisfaction typically dips in the first year postpartum for most couples and recovers. Communication is more important than agreement — the couples who talk about the difficulty cope better than those who perform okay-ness.
Sex after birth
The standard medical clearance is 6 weeks after a vaginal birth or C-section. However:
- Physical readiness at 6 weeks does not equal emotional readiness
- Many women need 3–6 months before sex feels comfortable or desired again
- Low libido after birth is driven by oestrogen suppression (breastfeeding keeps oestrogen low), fatigue, physical discomfort, and the identity shift of new motherhood — it is not a permanent change
- Pain with intercourse (dyspareunia) is extremely common, particularly after perineal tears. Vaginal dryness from low oestrogen makes this worse — use lubricant. If pain persists beyond 3 months, see a gynaecologist or pelvic floor physiotherapist
- Communicate with your partner. Set realistic expectations. There is no timeline that couples “should” return to sex.
Frequently Asked Questions
Q: My lochia (postpartum bleeding) stopped at 3 weeks. Then it came back at 5 weeks. Should I worry?
A return of bleeding after it has stopped can indicate you have returned to activity too quickly, or occasionally signals a retained placental fragment. If the bleeding is light and settles within a day, it is likely activity-related. If heavy (soaking a pad in an hour), accompanied by fever, or foul-smelling, see your doctor promptly.
Q: I had a C-section. When can I drive?
At least 6 weeks, and only when you can perform an emergency brake without pain or hesitation. Some women need 8 weeks. Check with your doctor, and check your car insurance — some policies require medical clearance before driving post-surgery.
Q: I feel nothing for my baby. I thought I would be overwhelmed with love but I mostly feel numb and scared. Am I a bad mother?
No. The immediate rush of bonding love portrayed in films does not happen for everyone. For many mothers, bonding develops gradually over weeks. If numbness persists beyond 2–3 weeks, combined with low mood, withdrawal from the baby, or inability to respond to the baby’s cues, this is postpartum depression. Please speak to your doctor or a counsellor. The fact that you are asking this question suggests you care deeply about your child.
Q: Is it normal to still look pregnant at 3 weeks postpartum?
Yes. The uterus takes 6–8 weeks to return to its pre-pregnancy size. The abdominal muscles and skin have been stretched for 40 weeks. The postpartum body does not spring back. Do not compare yourself to celebrities who post flat stomach photos at 3 weeks postpartum — those images are either exceptional outliers, filtered, or achieved through practices that are harmful to postpartum recovery.
Q: My mother-in-law wants me to eat only specific foods and not leave the house for 40 days. I am feeling isolated and depressed.
Isolation is a risk factor for PPD. If the chilla restrictions are making you feel trapped and depressed, you need to speak up — to your partner, to your doctor, or to a trusted family member. Protecting the spirit of the chilla (rest, support, good nutrition) while refusing restrictions that harm your mental health is not disrespectful to tradition. Your mental health directly affects your baby.
Q: I am 3 months postpartum and still leaking urine when I sneeze. Is this permanent?
Almost certainly not, but it will not resolve without targeted treatment. Stress urinary incontinence is the most common postpartum physical complaint and the most under-treated. Pelvic floor exercises (consistent practice for 12–16 weeks) resolve mild to moderate leakage in most women. If they do not help, see a women’s health physiotherapist for an individualised programme. Do not accept leaking urine as “normal after having a baby.”