RED FLAG Symptoms That Always Need a Doctor
Go to the ER immediately if your child has any of the following:
- Difficulty breathing: ribs showing with each breath (retractions), nostrils flaring, breathing rate over 60/min in infants or over 40/min in older children, blue/grey lips or fingertips
- High fever in a newborn: any fever (temperature ≥ 38°C) in a baby under 3 months — go to emergency, do not wait
- Fits/seizures: any convulsion, stiffening, or uncontrolled shaking
- Altered consciousness: child is unusually difficult to wake, confused, limp, or unresponsive
- Signs of severe dehydration: no urine for 8+ hours, sunken fontanelle (soft spot on head), sunken eyes, no tears when crying, very dry mouth
- Purple or non-blanching rash: press a glass against the rash — if it does not turn white under pressure, this may be meningococcal disease. Go to emergency immediately.
- Projectile vomiting in a newborn: forceful vomiting after every feed in a baby 2–8 weeks old
- Neck stiffness with fever: child resists bending chin to chest
- Severe abdominal pain that does not resolve, especially on the right side
- Any injury to the head followed by vomiting, drowsiness, or unequal pupils
Fever
What is a normal temperature?
- Normal: 36.5–37.5°C
- Low-grade fever: 37.5–38°C
- Fever: ≥ 38°C
- High fever: ≥ 39°C
The most accurate methods by age:
- Under 3 months: Rectal thermometer (gold standard). Axillary (armpit) temperatures run 0.5°C lower.
- 3 months–4 years: Rectal, temporal (forehead), or tympanic (ear) thermometers.
- Over 4 years: Oral or tympanic.
Forehead strip thermometers and back-of-neck touching are not reliable. Invest in a digital thermometer — they are inexpensive and accurate.
Fever in a baby under 3 months: always a doctor visit
Fever in a newborn or young infant (under 3 months) is a medical emergency until proven otherwise. Young babies cannot localise infection — a fever can be the only sign of a serious bacterial infection (sepsis, meningitis, urinary tract infection). Do not give paracetamol and wait. Go to the hospital.
Paracetamol dosing by weight
Paracetamol (acetaminophen) is the recommended first-line fever treatment in India. The correct dose is 10–15 mg per kg of body weight, given every 4–6 hours as needed. Maximum 5 doses in 24 hours.
| Child’s weight | Paracetamol dose (120 mg/5 ml syrup) |
|---|---|
| 4–5 kg | 2 ml (48 mg) |
| 6–7 kg | 2.5 ml (60 mg) |
| 8–10 kg | 4 ml (96 mg) |
| 11–15 kg | 6 ml (144 mg) |
| 16–20 kg | 8 ml (192 mg) |
| 21–25 kg | 10 ml (240 mg) |
Ibuprofen (5–10 mg/kg/dose) is a safe alternative for children over 6 months, but avoid in children who are dehydrated, have kidney problems, or are vomiting. Do not alternate ibuprofen and paracetamol routinely — use one, not both.
Do not give aspirin to children under 16 — risk of Reye’s syndrome.
What fever is doing
Fever is the body’s immune response. A temperature of 38–39°C is not harming your child’s brain. The discomfort is worth treating, but bringing the temperature to exactly normal is not the goal. If your child has a 39°C fever but is playing and drinking normally, the illness is likely mild.
Febrile seizures
Febrile seizures occur in 2–5% of children aged 6 months to 5 years. They look terrifying — jerking, eye rolling, loss of consciousness for 1–2 minutes — but simple febrile seizures (less than 15 minutes, not recurring in 24 hours) do not cause brain damage and do not mean the child has epilepsy.
During a febrile seizure:
- Lay the child on their side (recovery position) on a soft surface
- Do not put anything in the mouth
- Do not restrain the movements
- Time the seizure
- Stay calm — it will stop on its own
Go to hospital after the seizure if: it lasts more than 5 minutes, the child does not return to consciousness within 30 minutes, or this is the first seizure. The doctor will assess for the cause of the fever.
When fever needs a doctor (beyond the ER criteria above)
- Fever lasting more than 3 days without a clear cause
- Child aged 3–6 months with fever ≥ 38.5°C
- Fever with rash (other than the common mild viral rash)
- Child who refuses all fluids for more than 8 hours
- Any fever where the parent feels something is seriously wrong (parental instinct matters)
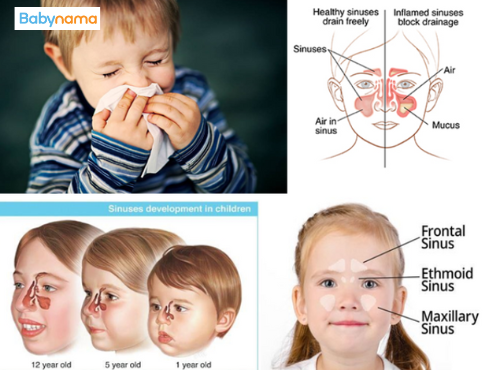
Cold and Cough
Babies and young children get 6–8 colds per year on average. This is normal. A child in daycare or with older siblings may get more. Each cold builds immunity.
What is normal
- Runny nose (clear, then yellow/green — colour change alone does not mean bacterial infection)
- Mild cough
- Mild fever for 2–3 days
- Reduced appetite
- Symptoms worse at night (mucus pools when lying down)
- Duration: 7–10 days
Home care that works
- Saline nasal drops: 2–3 drops in each nostril before feeds and sleep. This is the most evidence-based treatment for infant nasal congestion. Use commercially available saline drops (Nasivion, Nasoclear, Otrivin Baby) or make at home: 1/4 teaspoon of salt in 240 ml cooled boiled water.
- Steam inhalation: Sit with the baby in a steam-filled bathroom (run a hot shower) for 10–15 minutes. Do not use steam machines near the baby’s face — burn risk.
- Keep the head slightly elevated during sleep (raise the mattress end).
- Honey for cough (over 1 year): 2.5–5 ml of honey (half a teaspoon) before sleep. This has equivalent evidence to over-the-counter cough medicines in older children — and unlike OTC medicines, it is safe. Not before 1 year (botulism risk).
- Fluids: Breast milk, formula, warm water, soup. Hydration thins mucus.
What does NOT work (and can harm)
- OTC cough and cold medicines in babies under 2: These have been banned from use in under-2s in many countries and are strongly cautioned by CDSCO in India. They do not reduce symptoms and can cause serious side effects (seizures, irregular heartbeat, death in overdose).
- Antibiotics for a cold: Colds are viral. Antibiotics kill bacteria. Antibiotic misuse for colds has created the antibiotic resistance crisis India now faces. Yellow/green mucus alone is NOT an indication for antibiotics.
- Eucalyptus/camphor rubs on infants: Vicks VapoRub and similar products should not be applied to infants under 2 — menthol and camphor can cause respiratory distress. A baby-safe formulation (Vicks Baby Rub, eucalyptus-free) is available.
When cold needs a doctor
- Breathing difficulty: fast breathing, noisy breathing (not the congested snuffle), ribs visible with each breath
- Feeding refusal for more than 2 feeds in a young baby
- Fever lasting more than 3 days or recurrence after seeming to improve (may indicate secondary bacterial infection)
- Ear pulling + fever (ear infection — see below)
- Wheeze (a musical whistle on breathing out) — this may be bronchiolitis or viral wheeze and needs assessment
Diarrhoea
Diarrhoea is defined as 3 or more loose, watery stools in 24 hours — different from the baby’s normal. In fully breastfed newborns, frequent loose yellow stools after every feed are normal (not diarrhoea).
The single most important treatment: ORS
Oral Rehydration Solution (ORS) is the treatment. It replaces water and electrolytes lost in diarrhoea and prevents dehydration — the only reason diarrhoea kills. Antibiotics, anti-diarrhoeal medicines, and “gut rest” (stopping feeding) are all wrong. Keep feeding, start ORS.
Packaged ORS: Electral, ORS IP sachets (available at any pharmacy) — dissolve one sachet in 200 ml cooled boiled water. Do not add more water or juice to dilute it. Taste can be improved with a squeeze of lemon.
Home-made ORS (WHO formula): 1 litre of cooled boiled water + 6 level teaspoons of sugar + 1/2 teaspoon of salt. Stir until dissolved.
How much ORS to give:
- Under 2 years: 50–100 ml after each loose stool
- 2 years and over: 100–200 ml after each loose stool
- Offer small sips frequently — do not force large amounts at once (it triggers vomiting)
Zinc reduces severity and duration
WHO and IAP recommend zinc supplementation for all children with diarrhoea:
- 10 mg/day for infants under 6 months (Zincolac, Zinconia drops)
- 20 mg/day for children 6 months and above
- For 14 days — even after diarrhoea stops, zinc reduces the risk of recurrence
Keep feeding
Do not stop breast milk or formula. Do not give “gut rest.” Continue normal feeds. For older children, feed soft, easily digestible foods — dal rice, curd rice, banana, roti. The BRAT diet (banana, rice, applesauce, toast) is no longer specifically recommended but these foods are gentle and appropriate.
Danger signs requiring immediate medical attention
- Sunken eyes or sunken fontanelle (soft spot on head)
- No urination for 8 hours (a dry nappy for 8 hours is a red flag)
- Crying without tears
- Extremely lethargic or difficult to wake
- Blood in stool (dysentery — needs a stool culture and possible antibiotics)
- Persistent vomiting preventing ORS intake
- High fever with diarrhoea in infants
Vomiting
When vomiting is normal
- Posseting (small spills after feeds) in young babies — this is reflux, not vomiting
- Vomiting once or twice with a viral illness (cold, gastroenteritis)
- Vomiting with a high fever (this is common, not a separate emergency)
When vomiting is serious
- Projectile vomiting in a 2–8 week old baby: forceful vomiting that shoots out, occurring after most feeds, and worsening over days. This is pyloric stenosis (a narrowing of the stomach outlet) until proven otherwise. The baby will appear hungry, vomit, and then want to feed again immediately. This needs urgent ultrasound and likely surgical correction.
- Bile (green) vomiting in any baby at any age — suggests intestinal obstruction. Emergency.
- Blood in vomit — emergency.
- Vomiting with severe abdominal pain that does not settle — appendicitis, intussusception.
- Vomiting with high fever and neck stiffness — meningitis until proven otherwise.
For typical vomiting (gastroenteritis)
- Hold off feeds for 15–30 minutes after vomiting
- Offer small sips of ORS — 5 ml every 5 minutes to start
- Gradually reintroduce breast milk, formula, and soft foods
- If the child cannot hold down even small sips after 4–6 hours, go to hospital for IV fluids
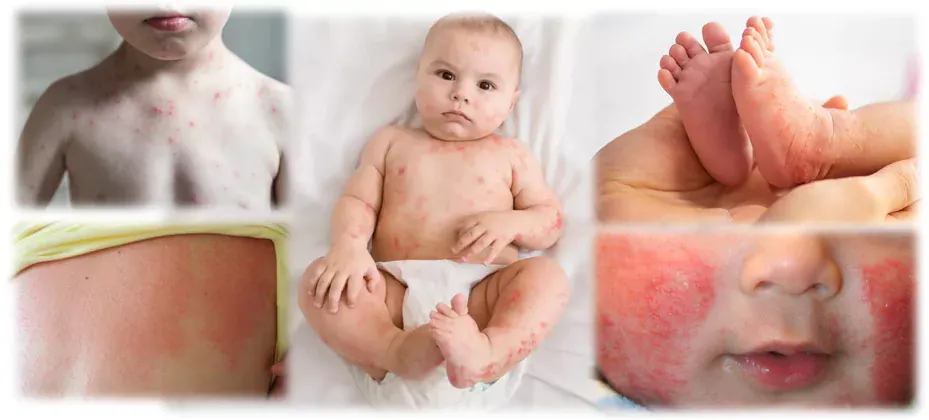
Rashes
Indian parents encounter many different rashes — most are benign, a few are not.
Benign rashes that do not need treatment
Heat rash (prickly heat / ghamori): Tiny red bumps, often on neck, back, and nappy area. Caused by blocked sweat glands in hot weather. Treatment: cool environment, loose cotton clothes, no talcum powder (which can be inhaled). Calamine lotion helps with itching.
Milia: Tiny white bumps on a newborn’s nose and cheeks. These are blocked sebaceous glands and resolve spontaneously in 4–8 weeks. No treatment needed.
Newborn acne (neonatal acne): Red pimple-like spots on the face in newborns, appearing at 2–4 weeks. Caused by maternal hormones. Clears by 3 months without treatment.
Erythema toxicum: A blotchy red rash with small white or yellow pustules, appearing in the first week of life. Benign, resolves in 1–2 weeks.
Viral rashes: Many common viruses cause a full-body rash as they resolve — particularly roseola (high fever for 3–5 days, rash appears as fever breaks) and hand foot and mouth disease (see below). These rashes typically look worse than they are.
Rashes that are serious
Petechiae: Tiny pin-point red or purple dots that do NOT blanch (turn white) when pressed. Petechiae can indicate thrombocytopenia (low platelets — dengue, ITP) or meningococcal septicaemia. Any non-blanching petechial rash with fever is an emergency.
Purple/purpuric rash (meningococcal): A rash that looks like bruising or blood under the skin, often starting as small spots and rapidly spreading. This is meningococcal septicaemia — one of the most time-critical medical emergencies in paediatrics. If in doubt, go to ER immediately.
Hives (urticaria) with breathing difficulty or facial swelling: This is anaphylaxis. Emergency.
The glass test for rashes
Press a clean glass tumbler firmly against a red or purple rash. If the rash turns white (blanches) under pressure, it is likely benign (blood is being displaced). If it stays red or purple under the glass (non-blanching), it may be petechiae or purpura — seek emergency care.
Ear Infections
Signs in pre-verbal babies
Ear infections are common in young children — the Eustachian tube connecting throat to middle ear is short and horizontal in infants, making drainage poor. Signs include:
- Pulling or tugging at one ear
- Increased crying, especially when lying flat or feeding
- Fever
- Disturbed sleep
- Drainage from the ear (if the eardrum has perforated — this is painful but actually provides relief of pressure)
You cannot diagnose an ear infection at home. The only way to confirm is with an otoscope (ear examination). Many things cause ear pulling — teething, for example.
The India-specific problem with ear infections
There is a widespread practice in India of using antibiotic ear drops (Sofradex, Otosporin, neomycin-based drops) without diagnosis. These drops can cause hearing damage if the eardrum is perforated. Never put any drops in the ear without a doctor confirming the eardrum is intact.
Most acute otitis media in young children resolves without antibiotics. IAP guidelines recommend a “watchful waiting” approach for mild cases in children over 2 years. Antibiotics are indicated for children under 2, severe cases, and recurrent infections.
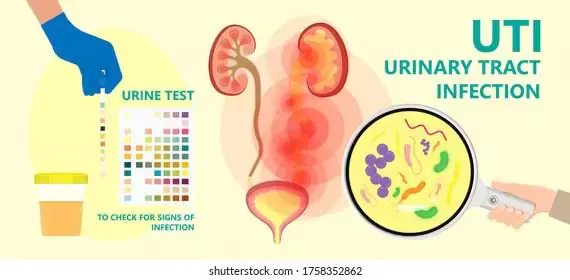
Urinary Tract Infections (UTI)
UTI is one of the most commonly missed diagnoses in young Indian children, particularly girls. The urinary tract is the second most common site of bacterial infection in babies after the respiratory tract.
Why it is missed
- Young babies cannot say “it hurts when I wee”
- The only signs may be: fever without obvious cause, irritability, poor feeding, vomiting
- Many doctors do not test for UTI unless prompted
Symptoms by age
- Under 2 years: Non-specific — fever, irritability, poor feeding. Occasionally, the parent notices the baby winces or cries when urinating.
- 2–5 years: May start saying “pain down there,” frequent urination, bedwetting after being dry, cloudy or foul-smelling urine.
- Older children: Burning urination, frequency, lower abdominal pain, fever (if kidney infection).
Why it matters
Untreated or delayed UTI in infants can lead to kidney scarring (reflux nephropathy), which can cause chronic kidney disease in adulthood. A urine culture is not optional when UTI is suspected in a young child.
If your baby under 2 has fever for more than 2 days with no obvious cause, ask your doctor to test the urine. A clean-catch or catheter urine sample, sent for culture, is the standard. Urine dipstick alone can miss UTI in young children.
After the first UTI, most children need an ultrasound of the kidneys and bladder (renal sonography). Some children have vesicoureteral reflux (VUR), where urine flows backwards from bladder to kidney — this needs specific management.
Hand Foot and Mouth Disease (HFMD)
HFMD is a highly contagious viral illness caused by Coxsackievirus and Enterovirus, common in India especially during monsoon and post-monsoon months. Daycares and nurseries are hot spots.
Symptoms
- Fever for 1–2 days
- Sore throat and mouth ulcers (on the tongue, gums, inner cheeks — very painful, can cause feeding refusal)
- Blister-like rash on palms, soles, and buttocks (sometimes the face and elsewhere). The rash is not itchy — this distinguishes it from chickenpox.
- Total illness: 7–10 days
Management
- Paracetamol for pain and fever
- Cold foods and fluids for mouth ulcer relief: cold yoghurt, ice lollies (if the child is over 1), cold milk
- Ensure adequate hydration — mouth pain makes drinking painful, dehydration is the main risk
- Keep child home from school/daycare for the duration of the illness (and until all blisters have dried/crusted)
No specific treatment or vaccine (in India)
There is no antiviral treatment. Antibiotics are useless. The EV-A71 vaccine is available in some countries but not yet in India’s routine schedule.
When to see a doctor: Persistent high fever, child who refuses all fluids for more than 6–8 hours, child who seems unusually drowsy or irritable (rare severe complications include viral encephalitis).
Dengue in Children
Dengue fever, transmitted by the Aedes mosquito, is endemic across urban India. Outbreaks peak post-monsoon (September–November). Awareness of warning signs can save lives.
Symptoms
- Sudden high fever (39–40°C), often “saddle-back” (dips, then rises again)
- Severe headache, especially behind the eyes
- Muscle and joint pains (“break-bone fever”)
- Rash: flushing early, then a measles-like rash appearing on day 3–5
- Nausea and vomiting
Warning signs of severe dengue (go to hospital immediately)
- Severe abdominal pain
- Persistent vomiting (3+ times in 24 hours)
- Rapid breathing or difficulty breathing
- Bleeding from any site: gums, nose, black stools, blood in urine
- Restlessness or sudden lethargy after a period of fever
- Cold, clammy skin (shock)
The platelet count myth
One of the most common misconceptions in India: that low platelet count requires platelet transfusion. This is not true. Platelet transfusion is only required for active serious bleeding or platelet count below 10,000/μL in a bleeding patient. A platelet count of 30,000–80,000 with dengue, no active bleeding, and stable vital signs does not automatically need hospitalisation or transfusion.
Daily platelet counts cause significant parental anxiety. Focus on hydration, feeding, and the clinical warning signs above.
Management
- Paracetamol for fever (NOT ibuprofen or aspirin — both increase bleeding risk)
- Good oral hydration: ORS, coconut water, nimbu paani, oral fluids
- Mosquito net or repellent to prevent reinfection and spread to family
When to Go to the ER: Clear Checklist
Go to the emergency room, not the pediatrician’s clinic, if your child has:
- Any fever in a baby under 3 months
- Difficulty breathing (fast breathing, retractions, blue lips)
- Seizure or fit
- Unresponsive or very difficult to wake
- Non-blanching rash (petechiae or purpura)
- Signs of severe dehydration (no urine 8 hours, sunken eyes, no tears)
- Projectile vomiting in a 2–8 week old
- Green (bile) vomiting at any age
- Neck stiffness with fever
- Dengue warning signs (severe abdominal pain, bleeding, shock)
- Suspected poisoning or ingestion of a foreign object
- Any situation where parental instinct says “this is serious”
Frequently Asked Questions
Q: My baby’s fever is 38.5°C. Do I need to go to hospital right now?
Age matters most. Under 3 months: yes, go immediately. Age 3–6 months: speak to a doctor or go to hospital. Over 6 months: 38.5°C with a child who is alert, feeding, and not showing any red flag signs can be managed at home with paracetamol and monitoring. The height of the fever matters far less than how your child looks and behaves.
Q: Should I alternate paracetamol and ibuprofen to control fever?
Not routinely. Each medicine given at the correct dose is effective. Alternating increases the risk of dosing errors. If one medication alone is not keeping the child comfortable and the fever is high (39.5°C+), alternating is sometimes used under medical guidance — but it is not standard first-line practice.
Q: My 9-month-old has had loose stools for 5 days. She is playful and drinking well. Should I worry?
Post-infectious diarrhoea (toddler’s diarrhoea) after a viral illness can last 2–3 weeks. As long as she is active, feeding, producing urine, and not showing dehydration signs, monitoring at home with ORS after loose stools is appropriate. If the diarrhoea is worsening, bloody, or she becomes less active, see a doctor.
Q: My child gets ear infections repeatedly. Is there anything I can do?
Breastfeeding significantly reduces ear infection risk. Avoid bottle feeding while lying flat. If infections are very frequent (4+ per year), the pediatrician may refer to an ENT for consideration of grommets (ear tubes) or adenoid assessment. Keep the child’s hands clean and reduce daytime exposure to large groups of children during cold season.
Q: Is it true that antibiotics are being overused in India and this is dangerous?
Yes. India has one of the highest rates of antibiotic-resistant infections in the world, partly due to over-the-counter antibiotic availability and over-prescription. Never pressure your doctor for antibiotics for a cold or routine viral illness. Finish the full course when antibiotics are genuinely needed. Do not use leftover antibiotics from a previous prescription. This matters for your child and for every child in the country.
Q: What vaccinations help prevent the illnesses in this guide?
The IAP immunisation schedule covers several illnesses mentioned here: pneumococcal vaccine (reduces ear infections and pneumonia), rotavirus vaccine (reduces severe diarrhoea), influenza vaccine (annual, reduces secondary bacterial infections), and Hib vaccine (reduces one form of meningitis). Ensure your child is up to date. See our Vaccination guide for the full IAP schedule.